What Are the First Signs of Perimenopause? My Early Symptoms Explained
- Gabriela Cabrera-Kimchi

- Apr 10
- 4 min read
Updated: 6 days ago
Most people associate perimenopause with obvious symptoms like hot flashes or irregular periods.
But in my case, I didn’t notice any clear symptoms at all.
Instead, the first signs showed up in my health data and trackers—long before I would have recognised anything physically.
In this post, I’m sharing what changed, and why early perimenopause can begin before you feel anything at all.
What is Perimenopause?
Perimenopause is the transition phase before menopause, when sex hormone levels—especially estrogen and progesterone—begin to fluctuate.
It can start years before menopause, often in your late 30s or 40s, and the earliest changes aren’t always obvious.
In some cases, like mine, you may not feel symptoms at all—at least not at first.
Can Perimenopause Start Without Symptoms?
Yes, perimenopause can begin before noticeable symptoms appear.
Hormonal changes often happen gradually, and in the early stages, they may only show up as subtle patterns—like shifts in sleep, cycle length variations, or other more subtle health data—rather than physical symptoms you can clearly feel.
That’s exactly what I experienced.
The First Signs I Noticed that are not obvious (Through Data, Not Symptoms)
I didn’t wake up one day feeling different.
But over time, my trackers started telling a different story.
I’ve been tracking my physiology using an Oura ring since 2022, so I know my baseline very well.
Recently, I started to see small but consistent changes:
Lower heart rate variability (HRV)
Slightly higher resting heart rate
Slower recovery
Reduced resilience
Lower temperature rises in my luteal phase
Nothing dramatic. But enough to tell me something had shifted — despite no changes in my lifestyle.
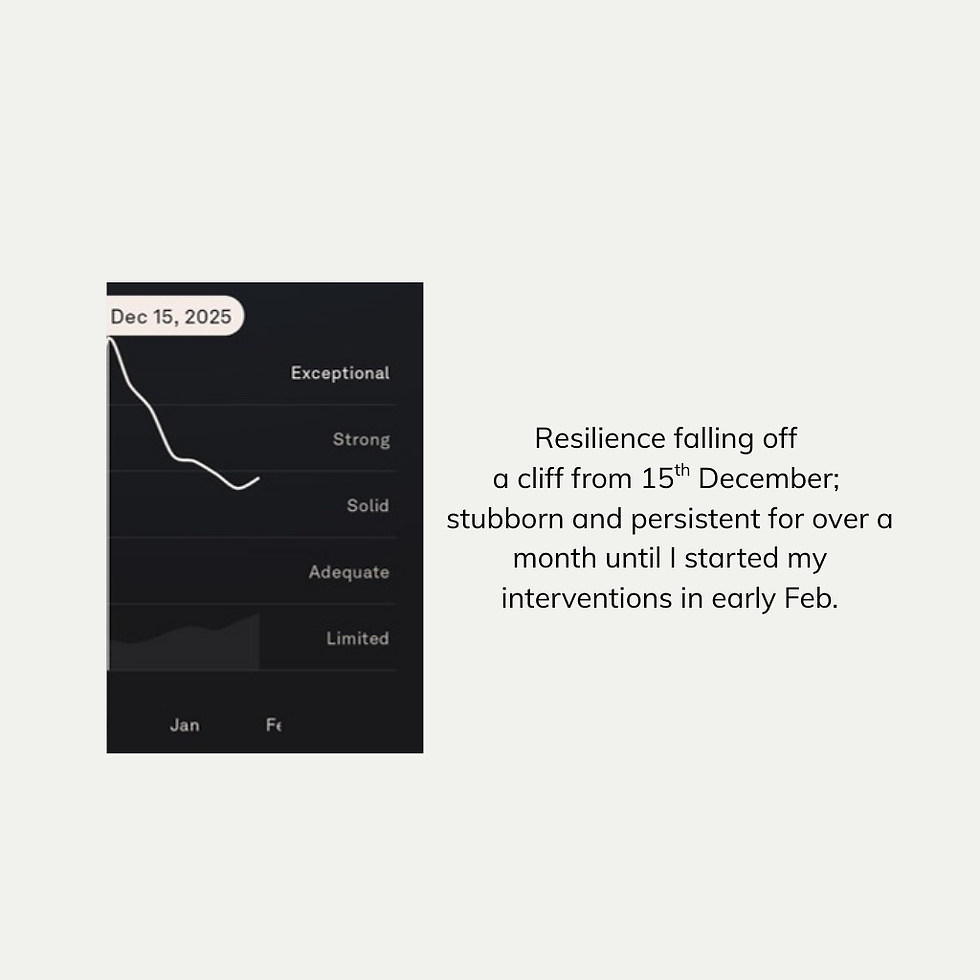
No hot flushes. No insomnia. No emotional symptoms.
Just less buffer.
And this is exactly what so many of my clients say to me:
“I just don’t feel like myself anymore.”
Not unwell. Not burnt out. Just… less steady. Less able to bounce back.
Why Resilience Drops in Early Perimenopause
One of the earliest hormonal changes in perimenopause is a decline in progesterone — not estrogen.
Progesterone is produced after ovulation, and as ovulation becomes less consistent in your 40s, levels can drop.
This matters because progesterone has a calming effect on the brain. It converts into allopregnanolone, which enhances GABA activity — your nervous system’s main “relaxation” pathway.
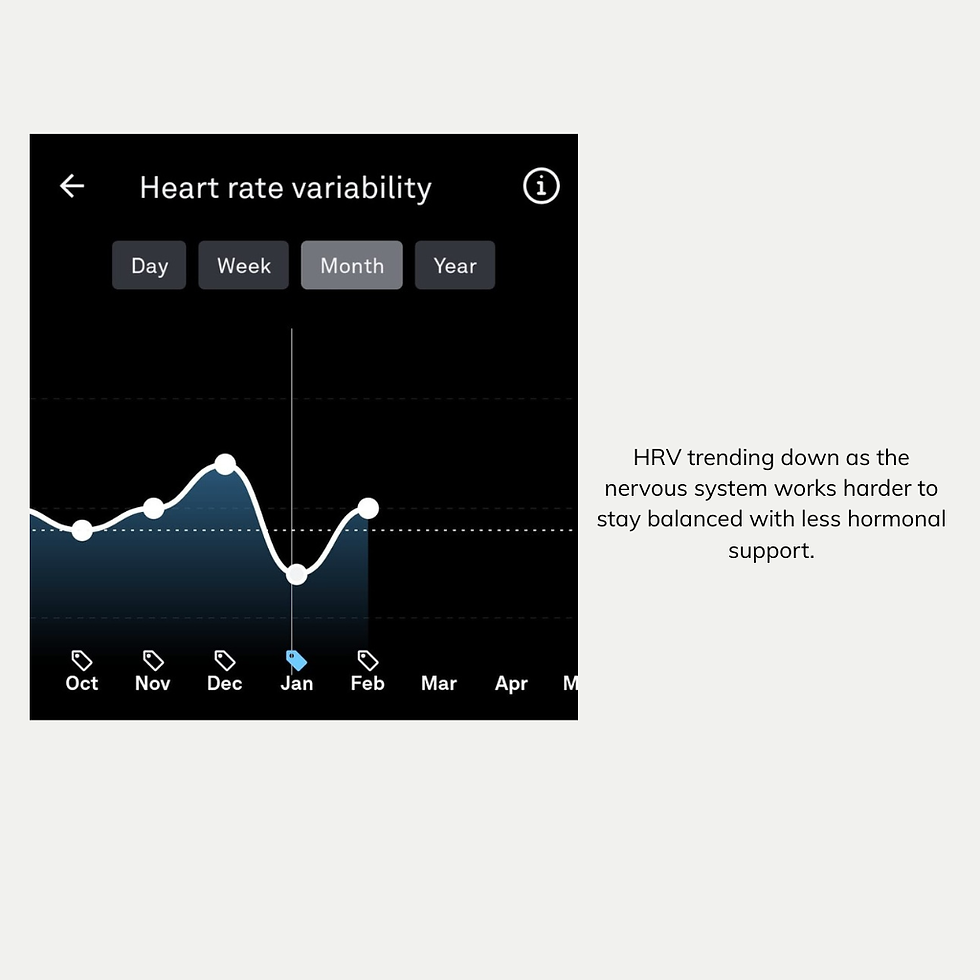
When progesterone declines:
The nervous system becomes more reactive
Stress feels more intense
Recovery slows
HRV often decreases
This is why so many women experience that subtle but persistent feeling of being “off.”
IN EARLY PERIMENOPAUSE, Estrogen Isn’t Low — It’s Unbalanced
Early perimenopause isn’t usually about low estrogen. It’s about unopposed estrogen.
As progesterone drops, estrogen can fluctuate or remain relatively high without balance.
This can lead to:
Lower stress tolerance
Unstable energy
Lighter sleep
A body that feels harder to predict
Why Tracking Your Hormones Matters
To confirm what I suspected, I used a Mira hormone tracker.
This allows you to measure hormone patterns at home, including:
LH (luteinising hormone) — helps identify ovulation
FSH (follicle-stimulating hormone) — can begin to rise as ovarian signalling changes
Progesterone (via PdG)
Estrogen (via E3G)
Together, this gives you a real-time picture of:
Whether you’re ovulating
Whether progesterone rises properly after ovulation
How estrogen behaves across your cycle
How your brain-to-ovary signalling is shifting
It’s a tool I use regularly in clinical practice — supporting women with fertility, PCOS, endometriosis, and perimenopause, and I am proudly a Mira-approved practitioner.
It’s incredibly insightful, and in my experience, an amazing tool for helping women truly understand their hormone patterns in real time.
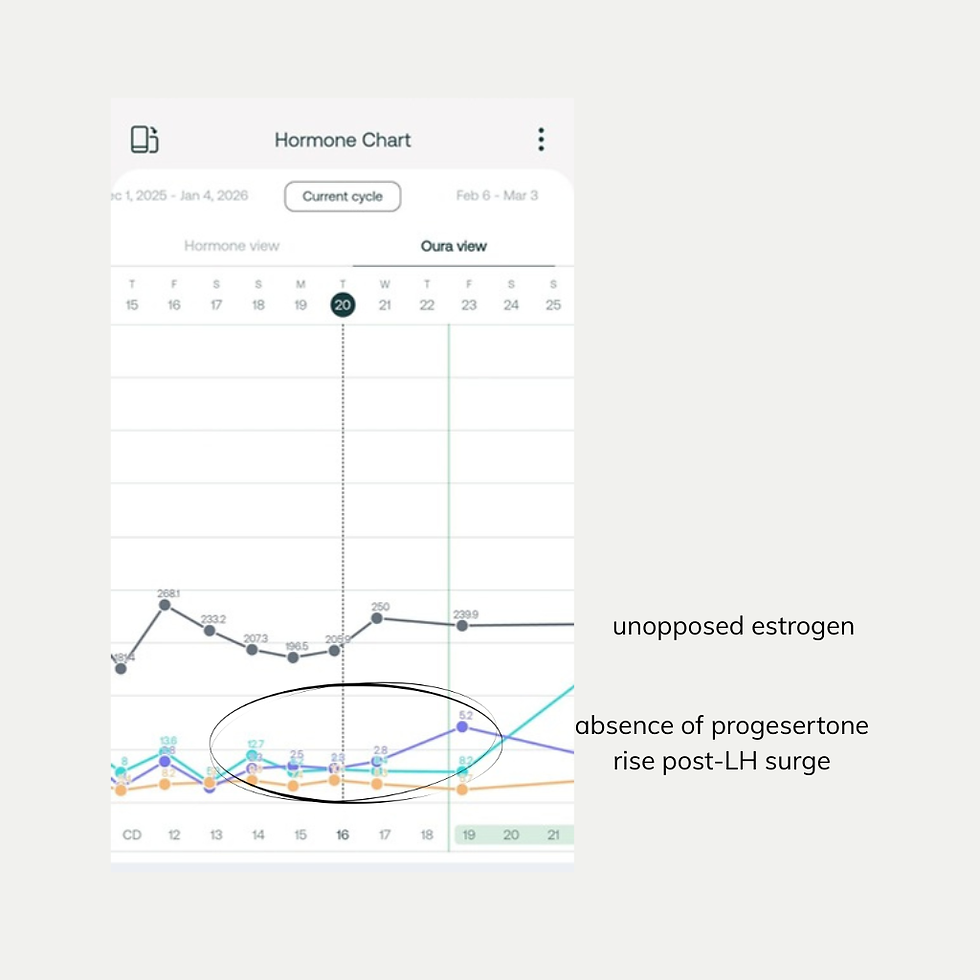
Within days, I saw:
Inconsistent ovulation
Low progesterone
Estrogen without proper balance
This confirmed early perimenopause — before symptoms appeared.
What I’m Doing to Support My Body
Perimenopause isn’t a problem to fix — it’s a physiological transition that can unmask underlying vulnerabilities, reduce resilience capacity, and calls for more personalised, tailored support.
Disclaimer: As a functional medicine practitioner, I’ve invested in extensive functional testing over the years and understand my own hormone patterns and physiology well. So the following approach is personalised and intentional and not something I would recommend copying blindly without context or professional guidance.
What I am doing:

1. Hormone Support (Carefully)
Low-dose pregnenolone (to support hormone production pathways)
Vitex to support ovulation and progesterone signalling
2. Nervous System First
Prioritising sleep
Avoiding overtraining
Building in more recovery
Supporting blood sugar balance
3. Botanical Support
Adding gentle plant-based support to help regulate the nervous system as progesterone declines.
4. Doubling-down on the Foundations
This is the non-negotiable layer — and often the most impactful.
Nutrient-dense, balanced meals
Consistent, quality sleep
Daily parasympathetic (rest-and-digest) activation
Regular movement with a focus on strength training (without overreaching)
Because in this phase, the basics aren’t basic — they’re everything.
The Key Takeaway
Perimenopause doesn’t always start with obvious symptoms.
Often, it begins with:
Lower resilience
Slower recovery
Feeling “not quite yourself”
You’re not imagining it. You’re not doing anything wrong.
Your body simply has less buffer than it used to — and that’s your signal to adjust support.
The Empowering Part
When you understand your body, you don’t have to wait for symptoms.
You can track. You can respond early. You can support your physiology before things escalate.
And that’s where real empowerment begins.
A Gentle Note From Me
If you’re reading this and thinking:
“What is actually going on with me?”
— you’re not alone.
Whether you’re curious about tracking with Oura or Mira,or you’re noticing that subtle shift and want help making sense of it…
I’m your girl.
Feel free to reach out — I’m always happy to help you understand your body a little better 🤍
When to Speak to a Doctor
If you’re noticing consistent changes—whether in how you feel or in your tracked data—it may be worth discussing them with a healthcare professional.
Tracking can help you spot patterns over time and have more informed conversations. Tools like Oura Ring and Mira Fertility Tracker generate reports that you can share with your practitioner for further interpretation.
I also work with prescribing doctors and can refer clients to practitioners who specialise in hormone replacement therapy (HRT), if/when appropriate.
If you’re curious about using wearables to help you track, I’ve shared my links below with practitioner discounts:


Comments